
The State of Caregiving 2018
As the Baby Boom generation ages, 10,000 people turn 65 daily. For the first time in U.S. history, there are more than 50 million seniors. This trend is expected to continue until 2029, when the youngest Baby Boomers will turn 65 years old. A third of those older than 65 live alone, and half of the “oldest old” — those beyond 85 — are on their own at this late life stage.
The aging population, coupled with the high cost of senior living and in-home care, is driving a growing demand for family caregivers – a trend that is expected to continue through the next several decades and beyond.
This guide provides a comprehensive look at the state of caregiving in 2018, as well as information to help family caregivers move forward with practical tools they can use today.
The New Normal
A 2015 survey conducted by the National Alliance for Caregiving and AARP, Caregiving in the U.S., approximately 34.2 million Americans provided unpaid care to an adult age 50 or older in the last 12 months, while 43.5 million provided unpaid care to an adult or child during the same 12-month period. Other findings include:
- More than 8 out of 10 caregivers (82%) provide unpaid care for one other adult.
- 15% provide care for two adults.
- 3% provide unpaid care for three or more adults.
- 16.6% of Americans (39.8 million caregivers) provide care for an adult (age 18 or older) with a disability or illness.
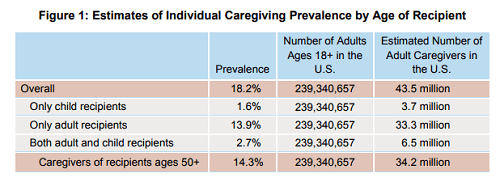
Graphic via Caregiving in the U.S.
In a new Merrill Lynch study, eight in ten Americans say caregiving is “the new normal.” While four in ten Americans 50+ believe they’re likely to need care at some point in their lives, the truth is, seven in ten Americans turning 65 today will need care for prolonged periods.
The price tag for informal caregiving is staggering: more than $500 billion. If these family members were replaced with skilled nursing care, the cost would jump to $642 billion annually. In fact, in 2013, the value of unpaid care exceeded the total value of Medicaid spending and paid home care in the same year – a total of $470 billion, an increase of $20 billion from 2009.
These numbers only continue to climb as the population ages. And aging it is, with the U.S. Census Bureau reporting that the number of U.S. residents age 65 and older reaching 49.2 million (15.2% of the population) in 2016, a rise from 35 million (12.4% of the U.S. population) in the year 2000. The median age is also increasing in many areas of the U.S. In 2016, two-thirds of all counties (66.7%) in the United States experienced an increase in median age, and two counties had median ages over 60:
- Sumter, Florida: 67.1 years
- Catron, New Mexico: 60.5 years
Between 2000 and 2016, nearly all counties (95.2%) across the U.S. experienced an increase in median age, with 56 counties having an increase in median age of 10 or more years. This trend is driven by a longer life expectancy: The average life expectancy in the U.S. was 68 years in 1950, rising to 79 years by 2013.
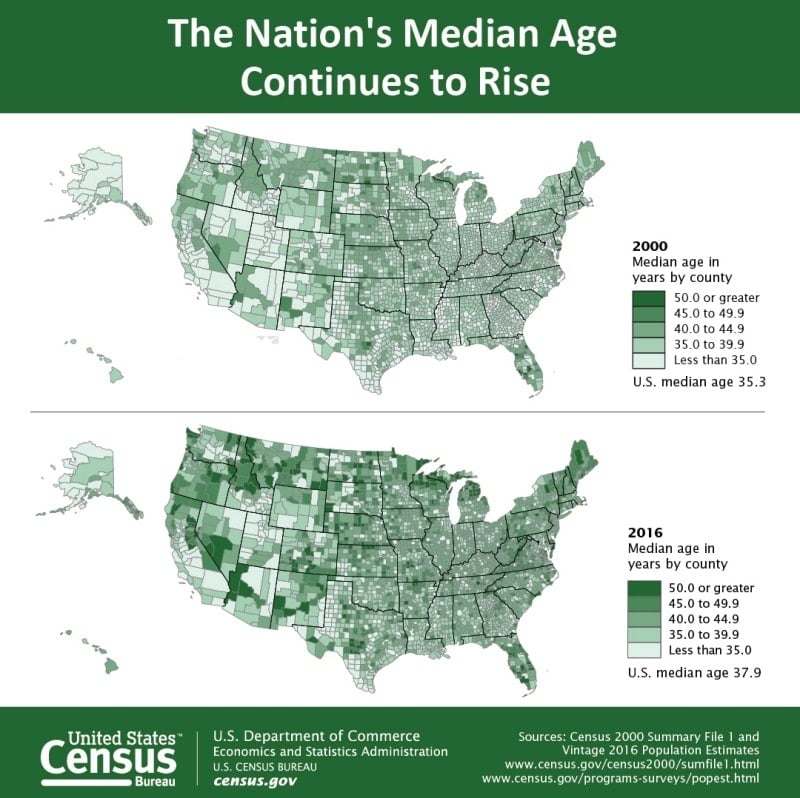
Graphic via U.S. Census Bureau
Who Are the Caregivers?
As the U.S. population is growing older, more Americans are finding themselves in a family caregiving role than ever before. According to the Institute on Aging (IoA), the average caregiver:
- Is female (75% of caregivers)
- Is 46 years old
- Is married
- Works outside the home
- Earns $35,000 annually
The prevalence of caregiving varies among demographic groups as well, such as race/ethnicity.

Graphic via Caregiving in the U.S.
Caregivers of adults are 49.2 years old, on average, but nearly half (48%) of all caregivers of adults are between the ages of 18 and 49. Caregivers who provide more hours of care per week tend to be older (an average of 51.8 years old) compared to those who provide less hours of care per week (48.0 years old). Overall, the majority of caregivers are adults between the ages of 45 and 64, with nearly one-fourth (23%) of adults in this age group caring for an aging adult. Nearly one in five (17%) of adults age 65 and older are caring for an aging adult, and among this group, 29% are providing care for a spouse or partner, while 33% are providing care for a friend or neighbor.
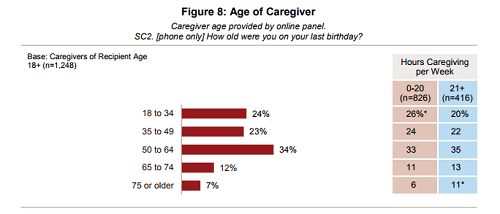
Graphic via Caregiving in the U.S.
Those who spend 21 or more hours each week providing care for a loved one are four times more likely to be caring for a spouse or partner, and the average age of spousal caregivers – 62.3 years of age – is higher compared to the average age of caregivers overall. One-fourth of caregivers spend 41 hours or more each week providing care, and those who live with their care recipient spend 40.5 hours per week providing care.
Caregivers spend, on average, thirteen days each month — more than 24 hours per week — on tasks such as shopping, food preparation, housekeeping, laundry, transportation, and giving medication. They spend another six days per month on tasks such as grooming, feeding, dressing, bathing, providing assistance with toileting, and other personal care needs, and they spend another 13 days each month researching care services or searching for information about disease, coordinating healthcare appointments, and handling financial matters.
A 2015 Pew Research survey asked respondents from the U.S., Italy, and Germany about the types of care they provided for an aging parent within the 12 prior months, finding:
- 60% of respondents with at least one parent age 65 or older have helped their aging parent with housework, home repairs, or running errands.
- 28% have helped an aging parent financially. Among this group, 43% say the financial assistance was for a recurring expense.
- 19% of female respondents say they provided personal care for an aging parent in the last 12 months (bathing, dressing, and similar tasks), while 8% of male respondents reported providing personal care assistance for an aging parent.
- 68% of respondents say they provide emotional support to an aging parent occasionally, while one-third say they do so frequently. (39% of female caregivers and 30% of male caregivers report providing frequent emotional support for an aging parent.)
Female caregivers in the U.S. spend about 50% more time providing care compared to their male counterparts, according to the IoA. There are also some differences in the care provided by female caregivers compared to male caregivers:
- Overall, female caregivers are more likely to provide personal care.
- 24% of male caregivers help their care recipient get dressed, compared to 28% of female caregivers.
- 16% of male caregivers help their care recipient with bathing, while 30% of female caregivers provide assistance with bathing.
- 4 in 10 male caregivers rely on paid assistance for some or all of their loved one’s personal care needs.
Of course, while these statistics paint a general picture of today’s caregivers, every situation is unique. Not only do care recipients have unique care and support needs, but family caregivers may differ in their approach to handling caring situations, as well. Two siblings, for instance, may share in the care of an aging parent, while in other cases, one primary caregiver provides most or all of the care for a loved one.
The Impact of Caregiving
While family caregiving may be a labor of love, true, it can exact a serious toll on the caregiver: physically, mentally, and financially. “Many caregivers put their own health and financial security at risk for the sake of their loved one. They often feel isolated at work or in their communities, unsure of where to go for resources or support,” explains AARP.
According to Richard Schulz, PhD and Paula R. Sherwood, PhD, RN, CNRN in a 2008 paper appearing in the American Journal of Nursing (AJN), “Caregiving has all the features of a chronic stress experience: It creates physical and psychological strain over extended periods of time, is accompanied by high levels of unpredictability and uncontrollability, has the capacity to create secondary stress in multiple life domains such as work and family relationships, and frequently requires high levels of vigilance.”
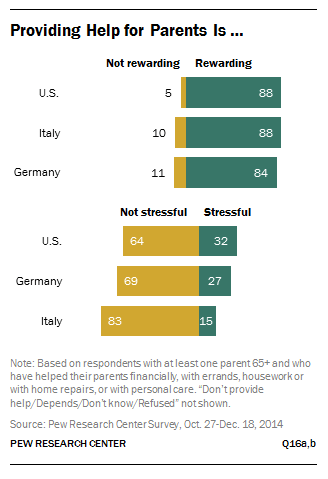
Graphic via PewSocialTrends.org
The impact of caregiving isn’t entirely negative, however. According to Pew’s research, 88% of adults who have provided financial help, personal care, or help with errands and household tasks to an aging parent say it’s rewarding. At the same time, nearly one-third (32%) say that helping aging parents with these tasks is stressful.
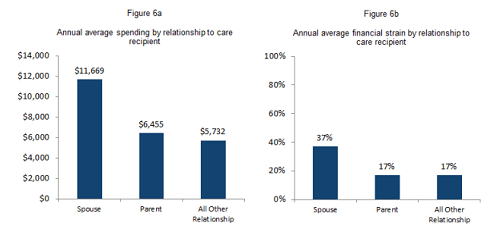
Financial stress is often a factor impacting family caregivers, as well. According to AARP’s Family Caregiving and Out-of-Pocket Costs: 2016 Report, 78% of family caregivers incur out-of-pocket costs. In 2016, family caregivers spent an average of $6,954 as a result of caregiving, typically about 20% of a caregiver’s income. The out-of-pocket costs caregivers incur is higher among those providing care for a loved one who requires assistance with two to six activities of daily living (ADLs) such as bathing and dressing, with this group spending an average of $10,236 out of pocket, compared to an average of $5,403 among those caring for a loved one who doesn’t require help with ADLs.
Graphic via AARP
Other financial factors include:
- The average out-of-pocket costs incurred by caregivers caring for someone with dementia was $10,697 in 2016.
- The average out-of-pocket costs incurred by caregivers who help with two to four medical or nursing tasks was $11,289 in 2016.
- Caregivers who do not provide assistance with medical or nursing tasks spend an average of $4,558.
- Hispanic family caregivers typically incur higher out-of-pocket costs, spending an average of $9,022.
- Long-distance caregivers (caregivers who live 1+ hours from their care recipient) also incur higher out-of-pocket costs: an average of $11,923.
- Spousal caregivers spend an average of $11,669, while caregivers providing care for an aging parent spend an average of $6,455 out of pocket.
- Caregivers between the ages of 71 and 91 spend more out of pocket ($13,875, on average) compared to caregivers between the ages of 51 to 70 ($5,486, on average).
Financial strain is compounded by work stress among family caregivers. Caregivers often have to take additional time off, either paid or unpaid, while some have to reduce their work hours. Others leave the workforce entirely in order to provide full-time care for a loved one.
Graphic via AARP
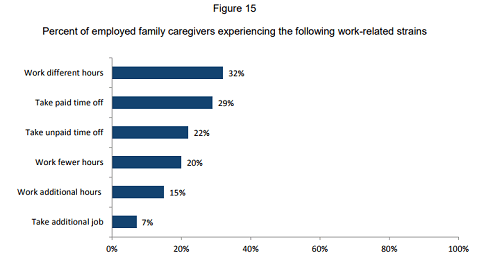
The most common work-related strains reported by caregivers include:
- 32% say they have to work different hours in order to meet caregiving obligations.
- 29% say they’ve had to take paid time off.
- 22% say they’ve had to take time off without pay.
- 20% work fewer hours in order to meet caregiving obligations.
- 15% say they work more hours in order to cope with the financial strain of caregiving.
- 7% say they’ve taken on an additional job in order to ease financial stress associated with caregiving.
More than one-third of family caregivers (35%) say that they’ve cut back on personal spending in order to meet caregiving expenses, and 30% of family caregivers say they’ve had to dip into their savings in order to cover caregiving-associated out-of-pocket costs. Additionally:
- 16% have reduced the amount they put into retirement savings.
- 14% have cut back on expenses related to their personal health.
- 11% have tapped into their retirement savings.
- 10% of borrowed money or taken out loans.
- 4% have retired early.
- 4% have had to resign from their jobs.
While economic status has an impact on the financial strain of caregiving, the difference is not as substantial as many may believe:
- 61% of low-income caregivers say they’re highly financially stressed.
- 34% of middle-income caregivers say they’re highly financially stressed.
- 40% of high-income caregivers say they’re highly financially stressed.
Caregiving also has an impact on the physical health of caregivers, with 17% reporting that they feel their general health has gotten worse. However, 72% of caregivers report that they don’t feel caregiving has had an impact on their own health.
Graphic via AARP
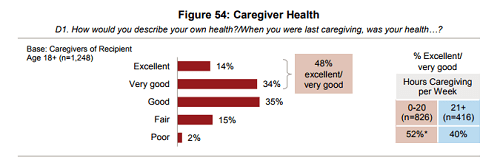
In general, the negative impacts on physical health tend to worsen over time, with 14% of caregivers reporting fair or poor health in the first year of caregiving, a figure that rises to 20% among those who have been providing care for five or more years. Spousal caregivers tend to feel these effects more than caregivers with other relationships to their care recipients: 27% of spousal caregivers report fair or poor health, compared to 15% of those with other relationships to their care recipients.
More than half of all caregivers (55%) report feeling overwhelmed by the amount of care their loved one needs. Accordingly, the portion of caregivers who report their own health as being fair or poor increases with the number of hours of care provided (22% of those who provide 20+ hours of care, compared to 14% of those providing 1 to 20 hours of care per week). Other physical and emotional impacts of caregiving include:
- Overall, 17 to 35% of caregivers rate their health as fair or poor.
- Between 40 and 70% of family caregivers caring for aging adults have clinically significant symptoms of depression. Among them, 25 to 50% meet the diagnostic criteria for major depression.
- 52% of family caregivers report that caregiving demands prevent them from spending time with other friends and family members.
- 19% report a high level of physical strain resulting from their caregiving duties, while 25% report a moderate level of physical strain. More than half of caregivers (54%) report little to no physical strain.
- 38% of caregivers perceive caregiving as “highly stressful.” One-fourth (25%) report moderate stress, while 36% say they feel little or no stress as a result of caregiving.
- Caregivers caring for a spouse or parent report higher stress compared to those caring for other friends or loved ones: 45% of those caring for a spouse and 44% of those caring for a parent report high stress levels.
Nearly all of these negative impacts affect a greater portion of caregivers who:
- Have a higher burden of care (e.g., their loved ones require more assistance with daily activities)
- Have been providing care for a longer time
- Are higher-hour caregivers (20+ hours per week)
- Are performing medical or nursing tasks
- Perceive a lack of choice in taking on a caregiving role
- Are caring for a loved one with Alzheimer’s disease or dementia, a mental health issue, or a long-term physical condition
On the other hand, nearly half of all family caregivers (48%) rate their health as very good or excellent. Those who provide 1 to 20 hours of care per week are more likely to rate their health as excellent or very good (52%) compared to those providing 20 or more hours of care per week (40%).
Dementia Care: A Daunting Scenario
Caregiving is challenging enough; when the person requiring care has memory loss, the problems are multiplied.
According to the Alzheimer’s Association, more than 5 million Americans are currently living with Alzheimer’s disease, and that number could reach more than 16 million by 2050. It’s currently the sixth leading cause of death in the United States. Among the top 10 leading causes of death in the U.S., Alzheimer’s disease is the only cause that “cannot be prevented, slowed, or cured.”

Screenshot via Alzheimer’s Facts and Figures
The growing prevalence of Alzheimer’s disease is a significant driver of the increased demand for family caregivers. More than 15 million people already provide unpaid care for a loved one with Alzheimer’s disease or dementia, accounting for an estimated 18.2 billion hours of care – a value of more than $230 billion.
Alzheimer’s disease is a multi-faceted, progressive disease that, over time, typically leaves a person unable to perform the typical tasks of daily living. While every individual is different, many people who suffer from the disease begin to require the help of a family caregiver for tasks such as keeping track of bills, household maintenance, and preparing meals, eventually relying on caregivers to help them bathe, get dressed, eat, and ambulate.
Caring for a loved one with Alzheimer’s disease or dementia carries a physical and emotional burden, often leaving caregivers feeling overwhelmed and stressed. Many family caregivers end up neglecting their own health and well-being, and as many as 30 to 40% of Alzheimer’s caregivers experience depression, high stress levels, or burnout. According to data from the Alzheimer’s Association, 35% of dementia caregivers say their own health has suffered as a result of their caregiving responsibilities – compared to just 19% of caregivers who are caring for a loved one without dementia.
How Caregiving Is Evolving
There’s increasing recognition among state and federal legislators of the growing demand for caregivers and the financial, physical, and emotional toll of caregiving, and while progress has been slow, there is some good news. The RAISE Family Caregivers Act, passed in late 2017 and signed into law in January 2018, “requires the U.S. Secretary of Health and Human Services (HHS) to develop, maintain and update an integrated national strategy to support family caregivers,” according to Richard Eisenberg in an article for Forbes.

Eisenberg explains, “Under the RAISE Act, HHS will create a national family caregiver strategy by bringing together federal agencies an representatives from the private and public sectors (like family caregivers, health care providers, employers and state and local officials) in public advisory council meetings designed to make recommendations. The agency will have 18 months to develop its initial strategy and then must provide annual updates.” Goals include addressing workplace policies that make it easier for family caregivers to continue working, training and respite options for caregivers, ways to increase financial stability, collecting and analyzing information about innovative family caregiving models, and assessing federal programs that serve the needs of family caregivers.
Aside from government efforts, a trio of aging experts recently weighed in on the need for alternate solutions as the longevity revolution alters Americans’ caregiving capacity.
Age Wave founder Ken Dychtwald, one of the nation’s foremost thought leaders on issues relating to an aging population; John Haaga, director of the Division of Social and Behavior Research at the National Institute on Aging; and gerontology professor Laura Sands, editor of the Gerontological Society of America‘s new journal, Innovation in Aging, offered this outlook for the future of caregiving:
- Apps and online tools to assist caregivers will proliferate. This is already happening.
- “Smart home” sensors will support caregivers and older adults who want to age in place.
- Universal design, which makes homes user-friendly as we age, will become the norm.
- “Care pathways” mapped on genetics, life and health preferences, and metadata analyses of whole populations vis-à-vis health interventions and outcomes, will improve.
- Robots, self-driving cars, and other forms of AI will lessen the load on human caregivers.
- Interdependence, in the form of retirement cohousing, the Village movement, intergenerational communities, and other ways to age together will become more common, helping to reduce isolation and loneliness, especially for “elder orphans.”
Technology to the Rescue

The rise in technological solutions to in-home care needs represents a tremendous boon for caregivers. From smart homes to robots, apps to digital diagnostics, “tech support” has never been stronger for the caregiving community. Millennials — often the grandchildren of those needing care — are at the forefront of these innovations, since they have a vested interest in ensuring their beloved grandparents are able to enjoy the best later life possible.
Some standout developments for caregiver support:
- Head in the Cloud. Developed in Belgium and now available stateside,Cubigo is a cloud-based, interactive platform that helps elders living at home remain independent and socially connected. Cubigo connects seniors, caregivers, family and businesses in an easy-to-use, modular interface. Users can order meals or transportation, monitor and share their personal medical data, setup medication reminders, and even order meals or transportation from a laptop, tablet, or smartphone with an internet connection.
- Driven to Serve Seniors. Transportation services such as Uber and Lyft could be problematic for seniors with mobility issues, or who are hearing impaired, for example. So one enterprising grandson created GoGoGrandparent, an on-demand ride service customized for older adults, with built-in monitoring. In addition to custom pickups and automatic scheduling for recurring rides (e.g., medical appointments), GoGoGrandparent provides by-the-minute text updates to designated family members.
- Bot Can They Play Bridge? Robots already play a valued role as automated housekeepers. Now they can also be companions for those with mild cognitive impairment. A care robot can remind a senior to drink enough water, take medication on time, and eat three meals a day. Robots can even act as surrogate friends: EllieQ is being designed to provide emotional support to seniors who want to age in place. The active aging companion keeps elders actively engaged. And yes, ElliQ can play bridge!
- The Perfect Pet. Virtual “pet companion”GeriJoy is a remote caregiving service that provides seniors who have mild dementia with an adorable animal avatar who will engage with the elder on demand, via tablet or laptop. GeriJoy’s remote caregivers are trained and compassionate, providing 24/7 monitoring services for aging adults. In the event of a behavior change or fall, GeriJoy alerts the designated emergency contact person.
When only the real deal will do, Hasbro has it handled, with Joy For All Companion Pets: animatronic “pets” that deliver tactile and auditory stimulation to seniors with dementia, providing comfort, care, and a calming influence — and they never need to be fed or walked.
It Takes A Village: New Model Supports Aging in Place
Even healthy seniors need help now and then, and as they grow older, the amount of help most seniors need increases. A caregiver might start out as a companion who assists with food shopping and laundry, and gradually assumes more hands-on caregiving as the senior ages or develops health issues.

Villages are one exciting new model that supports caregivers and seniors who want to age in place. They’re not physical structures, but hyper-local, member-driven, grassroots organizations that coordinate access to affordable services, and offer vetted (and often discounted) providers, complementing other community services. The more a Village grows, the broader the scope of services it’s able to provide.
Beacon Hill, a Boston neighborhood, developed the inaugural Village in 2001, and the concept mushroomed over the next decade. The Village-to-Village Network launched in 2010 to help communities establish and manage new Villages, and to grow the Village movement overall.
According to the Village-to-Village Network, “Village members experience reduced isolation, increased independence, and enhanced purpose of life.” Ilene Henshaw, Director of Health & Family, State Advocacy and Strategy Integration for AARP, says, “Villages are instrumental in helping people remain in their homes and independent in their communities.”
Currently, there are 230 Villages operating throughout the U.S., with 100 more in development. This map shows the ever-evolving status, and you can search by Village name, city or state to find one near you.
Becoming Your Best Self As A Caregiver: Tips and Traits
Patience and compassion are the bedrock of caregiving; anyone who has cared for another for any length of time probably embodies these attributes. However, there are several additional – and equally important – key traits:
- Awareness. People who become caregivers for their aging parents often find themselves facing behavioral changes. Sometimes seemingly overnight, or perhaps more gradually, a calm, loving parent becomes blunt, even mean — or possibly fearful. If it’s not a result of dementia or a change in their physiological state, the shift could signify frustration with the many-layered loss of control that tends to accompany aging.
An elder might be verbally or emotionally abusive to a caregiver with whom they feel safe enough to vent their pain or grief. Thank them for trusting you enough to be honest, back off from whatever you were doing/discussing, and don’t take it personally. It’s not about you.
- Tag team. Everybody needs support — especially caregivers. Whether it’s an Alzheimer’s chat board, mindfulness meditation training, or a relief caregiver so you have some much-needed time off, reach out to your community and put a network in place to help you avoid burnout. Lotsa Helping Hands is a web-based support community that enables caregivers to create a local support group.
- Smiles and Laughter. Humor helps lighten up even dire circumstances. If you have a music CD, TV show, video, or other go-to source that provides humor and relieves stress, be sure to make it a regular part of your life. The person you’re caring for will likely enjoy the laughter, too!
Remember, caregiving is a highly individualized journey, but talking with others who are going through similar experiences is a powerful support mechanism. Reach out to local resources and organizations to find out what services and options are available to you – don’t be afraid to reach out for help.
Caregiving Resources: Start Here
For more caregiving insights, resources, and tools to help you navigate the caregiving journey, visit the following resources:
- AARP – Housing Options and Home Care
- AARP – Benefits and Insurance
- AARP – Legal and Financial Issues
- AARP – Home-Based Palliative Care
- Family Caregiver Alliance – Legislation
- HHS.gov – Resources Near You
- Eldercare Directory – State Resources
- CMS.gov – What Caregiver Support Is Available In My Area?
- Family Care Navigator: State-by-State Help for Family Caregivers
- Mayo Clinic – Caregiver stress: Tips for taking care of yourself
- HelpGuide.org – Caregiver Stress and Burnout
- AgingCare.com – 10 Signs of Caregiver Stress
More insights like this:
-
Bradley Cooper’s Caregiving Reminds Us Who’s Really Holding Families Together
Read more: Bradley Cooper’s Caregiving Reminds Us Who’s Really Holding Families TogetherThe new documentary, Caregiving, comes at a critical moment. As Congress weighs major decisions that could impact families across the country for years to come, this film offers something powerful to inform those deliberations. It provides a window into the lives of family caregivers, and a lesson on the pivotal points in time…
-

Celebrating 25 Years of Supporting Family Caregivers
Read more: Celebrating 25 Years of Supporting Family CaregiversWhen Careforth began 25 years ago, it wasn’t just about launching a company. It was about showing up for families who were overwhelmed, unseen, and doing everything they could to care for someone they love at home. That belief—that family caregivers matter—has fueled every step of our journey since. Today, we celebrate a…
-

Careforth Expands Coordinated Caregiving Services Statewide in North Carolina
Read more: Careforth Expands Coordinated Caregiving Services Statewide in North CarolinaCareforth, a leading provider of caregiver support and resources, is expanding its family caregiving services to the entire state of North Carolina. Careforth’s comprehensive services provide financial assistance, expert coaching, and emotional support to caregivers of people of all ages. Having launched in 2020, we are currently serving hundreds of caregivers across the…